Auburn veterinary college, UAB part of joint NIH study of glioma brain cancer
Article body
People and animals suffering from the deadliest form of brain cancer are undergoing similar treatment in an NIH-funded clinical trial through the University of Alabama at Birmingham, Auburn University’s College of Veterinary Medicine and two other currently enrolled Southeastern veterinary programs.
Veterinarians and human medical doctors are collaborating on an NIH-funded clinical trial in which the same immunotherapy is being used to treat people and dogs with glioma, the most aggressive form of brain cancer. Dogs and humans develop malignant brain tumors at about the same rate and with similar biology.
Dr. Renee Chambers, who holds a doctor of veterinary medicine degree from Auburn and a doctor of medicine degree from UAB, has received funding from the National Institutes of Health for a multi-institutional consortium to evaluate immunotherapy for glioma tumors, the same type of brain cancer as the late Sen. John McCain.
CANINE (CANine ImmunoNEurotherapeutics) is a multicenter study to investigate immunotherapy for dogs with malignant brain tumors. Collaborators from around the country, including regional veterinarians at Auburn, Mississippi State and Georgia, are treating canine gliomas as part of this study. Treatment is entirely paid for by the study and includes surgery to remove all or most of the tumor, followed by treatment with a cancer-killing virus and checkpoint inhibitor in some cases, as well as all post-operative imaging, hospitalization and all scheduled postoperative visits.
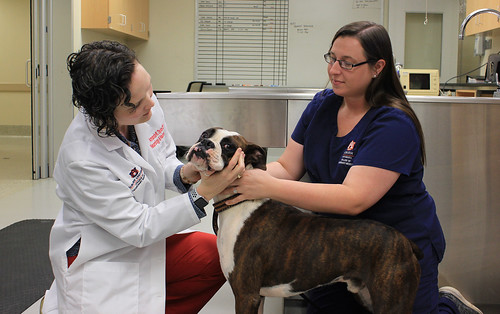
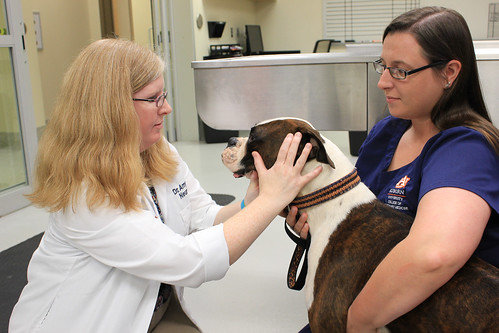
Auburn faculty Drs. Amanda Taylor and Amy Yanke, veterinarians who specialize in brain surgery, and Jey Koehler, a veterinary pathologist, are investigators in the clinical trial.
The oncolytic virus, M032, is a genetically engineered virus currently being used in FDA-approved human trials at UAB. In the canine trial, M032 is injected directly into the tumor bed shortly after surgery and can replicate in and destroy glioma tumor cells without affecting healthy brain cells. M032 also causes tumor cells to secrete an immune-stimulating protein, IL-12, before tumor cells die, which increases the anti-tumor immune response.
Dogs diagnosed with a suspected glioma brain tumor based on MRI imaging are eligible for enrollment in the study. Pet owners are responsible for costs of the initial referral exam and diagnostics leading to a brain tumor diagnosis.
“Through this clinical trial, dogs have access to incredibly sophisticated treatment and medicines,” said Koehler.
“This clinical trial is highly unusual in that the same treatment is being used in animals and people at the same time,” Yanke said. “We are at the forefront of medical treatment.”
At Auburn, dogs with suspected or diagnosed brain cancer will be seen by the Neurology and Neurosurgery Service at the Bailey Small Animal Teaching Hospital. With consent from owners, surgery will be conducted to remove all or part of the tumor. Histopathologic analysis will determine the exact type of brain tumor and, if a glioma, the dog can be enrolled in the trial.
Dog breeds that most typically are diagnosed with brain tumors include Boston terriers, French bulldogs and boxers. Brain tumor deaths are thought to be responsible for about 2 percent of cancer deaths in dogs.
Warning signs, according to Yanke, may include seizures, behavior changes, loss of vision and circling. “Some dogs are referred to us [by primary-care veterinarians] with signs.”
While not all pet owners enroll their pets in clinical trials, more and more owners are considering the treatment because of the quality of life for their pet and for the knowledge gained in a trial. “We are seeing clinical trials more often in both animal and human medicine,” Taylor said.
Koehler, who will oversee the pathologic diagnosis of the tumor, said another important part of the trial is looking at the immune response to the tumor. “An agent within the M032 [IL-12] is expected to stimulate the dog’s own immune system to help recognize and destroy cancer cells,” she said. “We are stimulating the immune system for it to recognize and destroy tumor cells to essentially help the body kill the tumor.”
Dogs and humans are among the few species that spontaneously develop naturally occurring brain tumors. Those tumors have a lot in common, too, which has led scientists at the NIH and at the University of Alabama at Birmingham to wonder whether studying tumors in dogs will help treat humans, and whether studying tumors in humans will help treat canine patients.
“Brain tumors in dogs and humans are remarkably similar,” said Chambers. “They share similar rates of incidence and morbidity and mortality, and they share similar symptoms such as seizures, which is often the first symptom observed in both humans and dogs. Treatment is very much the same, too, with surgery, radiation and chemotherapy the standard of care.”
Chambers, who was trained as a veterinarian prior to becoming a physician neurosurgeon, brings a unique perspective on the link between human and canine tumors.
“There are many shared factors between people and their pet dogs,” she said. “Dogs live in our houses, sharing the same environment and the same sleep patterns, for example. Some lucky dogs even share a diet with their owners. The tumors have similar gross and histopathologic characteristics. It is not unreasonable to assume that the dog will be a highly useful model of human brain tumors.”
“We anticipate that M032 will be as safe and effective in dogs as it has proven to be in humans,” Chambers said. “It opens up an exciting new research pathway, while providing the potential of a therapy that could benefit both humans and dogs with brain tumors.”
The five-year, $2.6 million project is funded by the Moonshot Initiative through the Center for Cancer Research of the NIH’s National Cancer Institute. The goal is to treat about 15 dogs per year at Auburn and the other participating veterinary schools.
“The hope is that this research will benefit both dogs and people,” Chambers said. “Given the relatively short lifespan of the dog compared to a human, the timetable for results is accelerated.
“We talk of ‘translational medicine,’ moving research from the laboratory bench to the hospital bedside. This project is a revolution in the approach, also translating research findings from human to animal and back to human, to the benefit of both.”
Related Media
Related Links
More Information
About M032
M032, a second-generation oncolytic herpes simplex virus derivative of G207 and M002, all developed in the laboratory of UAB neurosurgeon Dr. James Markert has been designed to infect tumor cells while leaving healthy cells alone. It replicates in and kills tumor cells. As the tumor cell dies, progeny viruses are released from the cell. These viruses infect other tumor cells in the vicinity and continue the process of tumor killing. But M032 also has a secret weapon—the virus was engineered to carry the human gene for interleukin-12, a powerful protein that stimulates and activates killer T-lymphocytes that are part of the patient’s own immune system.
Markert and Chambers, together with Dr. Yancey Gillespie, director of the UAB Brain Tumor Specialized Program Of Research Excellence, or SPORE, have been studying viral therapies for brain tumors for over 20 years. They first published a comparison of genetically engineered herpes simplex viruses for the treatment of brain tumors in a scid mouse model of human malignant glioma in the Proceedings of the National Academy of Science in 1995 and continue to study translational models to improve treatments and outcomes in patients diagnosed with a brain tumor.
Media interested in this story can contact Communications Director Preston Sparks at (334) 844-9999 or preston.sparks@auburn.edu.
The College of Veterinary Medicine is the South's original and nation's seventh oldest veterinary medical program, celebrating 126 years. We prepare individuals for careers of excellence in veterinary medicine, including private and public practice, industrial medicine, academics, and research. The college provides programs of instruction, research, outreach, and service that are in the best interests of the citizens of the state of Alabama, the region, the nation, and the world.